Introduction
Atrial hypertrophy, characterized by the enlargement of the heart's chambers, is a condition that is becoming increasingly common and poses significant risks to cardiovascular health. As healthcare professionals work to enhance patient outcomes, it is crucial to understand the causes, diagnostic techniques, and management strategies associated with this condition.
With the rising prevalence of obesity, diabetes, and sedentary lifestyles, clinicians face the challenge of effectively identifying and addressing the underlying factors that contribute to atrial hypertrophy.
This article explores the complexities of atrial hypertrophy, providing insights into its clinical significance and the latest advancements in diagnosis and treatment.
Define Atrial Hypertrophy and Its Clinical Significance
Enlargement of the heart's chamber areas, often due to prolonged pressure or volume overload, is a common condition that poses significant clinical challenges. This enlargement can lead to , such as irregular heartbeat and heart failure. For healthcare professionals, is crucial, as it signals underlying cardiac problems and influences treatment strategies.
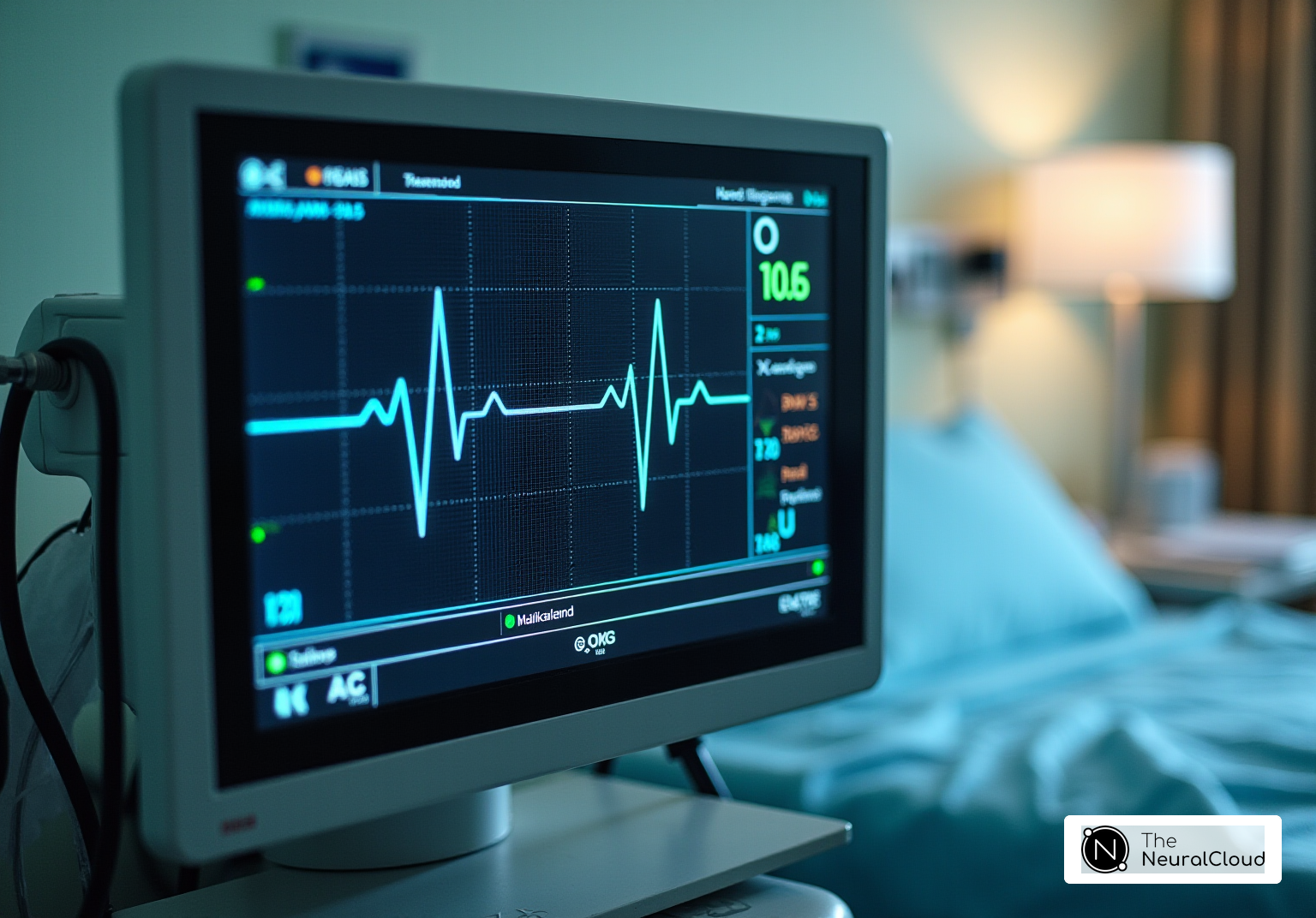
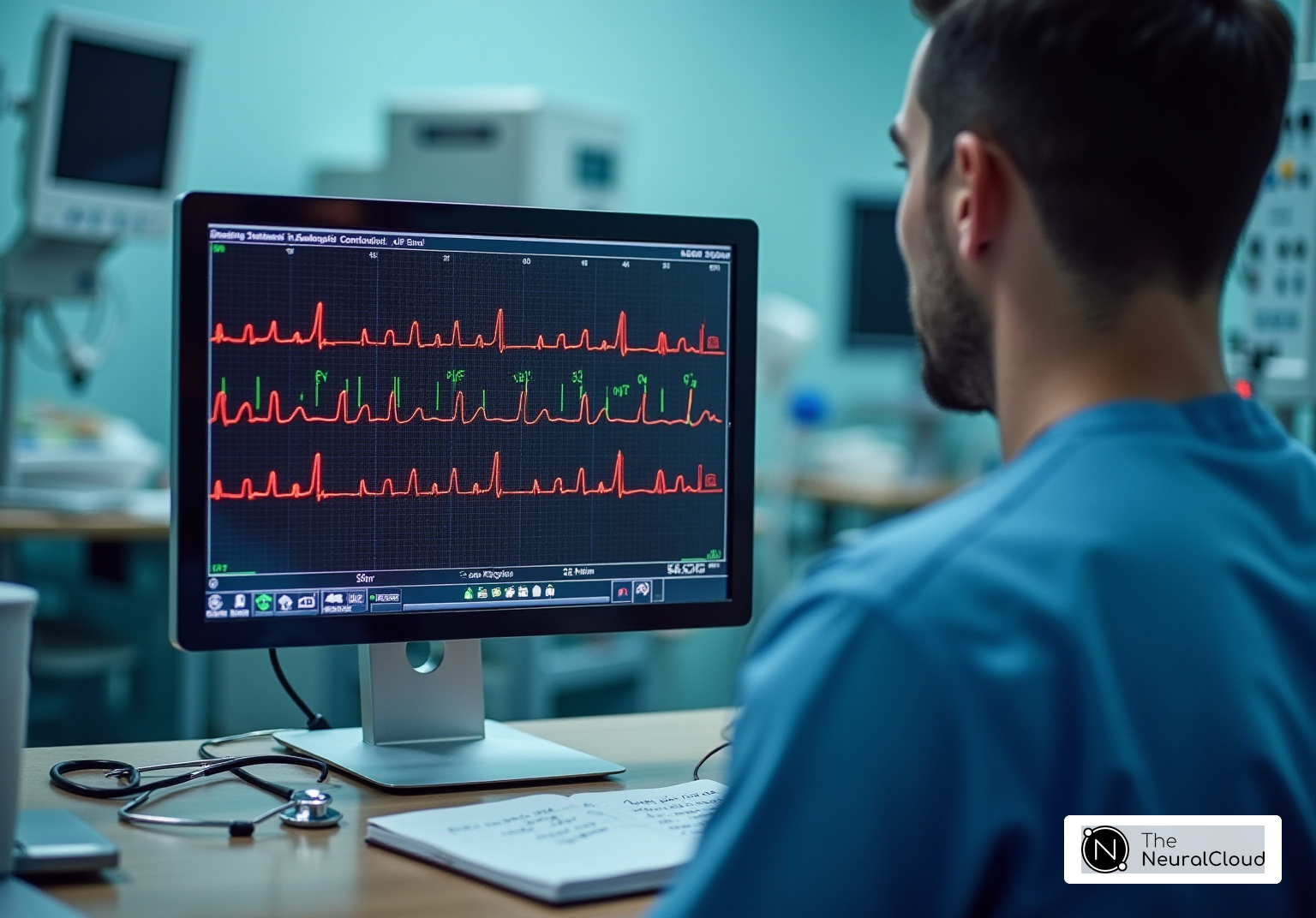
are essential diagnostic tools that reveal distinct changes in chamber size and function, allowing for timely intervention. However, traditional ECG interpretation can be hindered by , which obscure critical data. This is where Neural Cloud Solutions' comes into play.
Features of MaxYield™:
- Advanced noise filtering
- Distinct wave recognition
- Rapid isolation of ECG waves from recordings affected by baseline wander, movement, and muscle artifact
MaxYield™ enhances by salvaging previously obscured sections of lengthy Holter, 1-Lead, and patch monitor recordings. The algorithm evolves with each use, continuously improving its accuracy and efficiency in pursuit of maximum diagnostic yield.
Statistics show that is associated with increased mortality and morbidity, making its detection vital in clinical practice. Patients with LAE often present symptoms like breathlessness and fatigue, underscoring the need for regular monitoring and management. Understanding the implications of not only aids in but also elevates the overall quality of cardiovascular care.
Doctors must investigate the underlying causes of LAE to help individuals manage symptoms and enhance their quality of life.

Explore Causes and Risk Factors of Atrial Hypertrophy
can occur due to various underlying conditions, such as , valvular heart disease, and . Key , diabetes, and a . For example, the has increased significantly, with rates climbing from 32.5% to 60.4% among those with heart failure between 1988 and 2023. This trend underscores the critical link between obesity and , as excess weight can elevate filling pressures in the heart, resulting in compensatory growth in the chambers.
Diabetes also significantly impacts this issue. Studies show that only 25% of individuals with hypertension, hyperlipidemia, and diabetes manage to control all three conditions effectively. This lack of control can heighten the risk of developing atrial hypertrophy, as contribute to cardiovascular complications. Furthermore, a sedentary lifestyle exacerbates these risks, with physical inactivity linked to increased body weight and poor metabolic health.
Real-world examples highlight these connections: patients with a history of obesity and diabetes often report symptoms like fatigue and palpitations, which may signal underlying atrial hypertrophy in the heart muscle. Recognizing these risk factors is vital for early intervention and management. Addressing them can significantly reduce the incidence of atrial hypertrophy and its associated complications, such as heart rhythm disorders and cardiac failure. By focusing on - like regular exercise and dietary modifications - along with , healthcare providers can help mitigate the risks associated with heart muscle enlargement.

Discuss Diagnostic Techniques for Atrial Hypertrophy
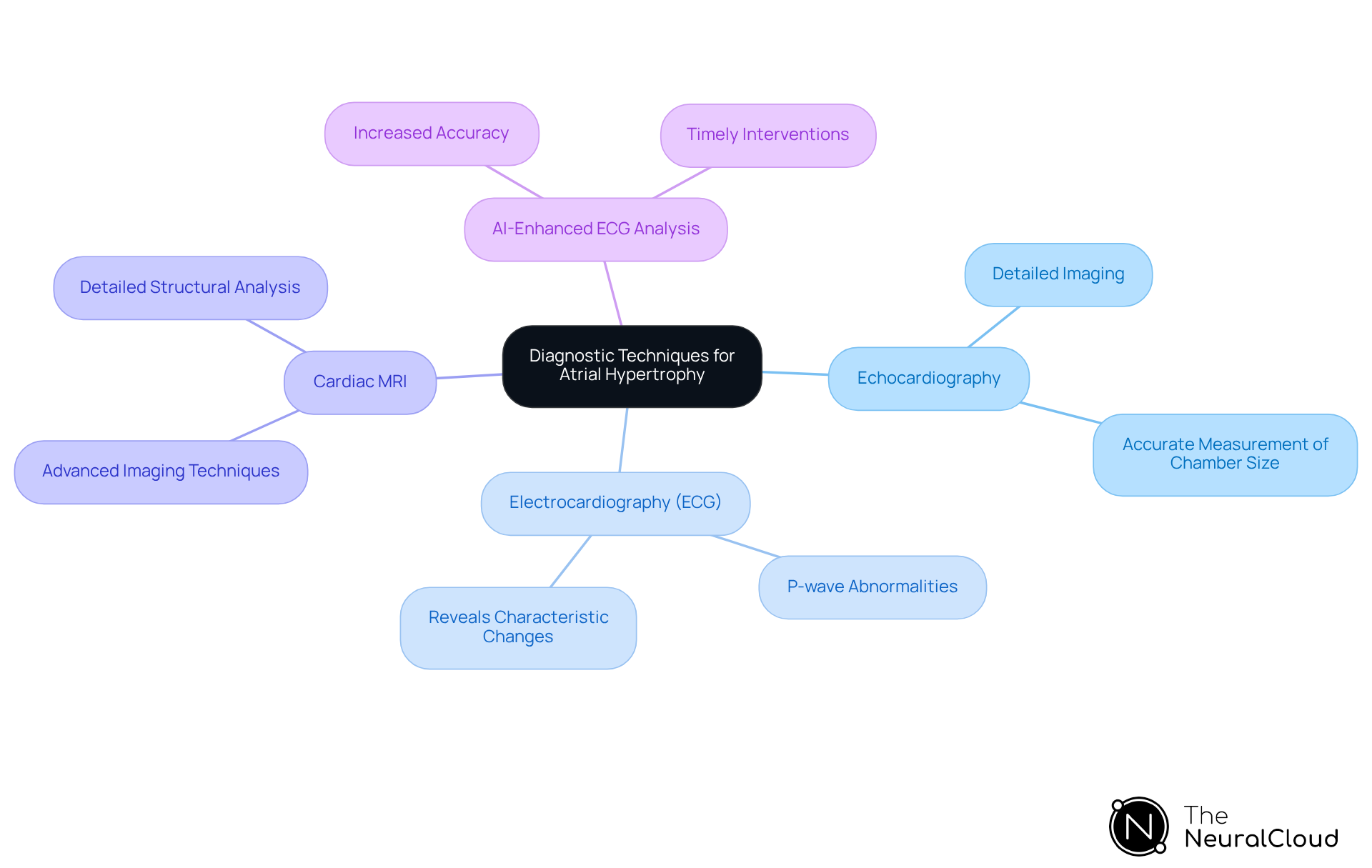
for heart muscle thickening primarily include echocardiography and . of the heart's structure and function, enabling accurate measurement of chamber size. This measurement is crucial for diagnosing conditions like . Meanwhile, ECG is essential as it reveals , particularly through P-wave abnormalities. Statistics indicate that a significant percentage of patients with heart muscle enlargement exhibit these ECG changes, underscoring the importance of this diagnostic tool.
Emerging technologies, such as cardiac MRI and , are transforming the diagnostic landscape. and efficiency in identifying structural changes, facilitating timely interventions. For instance, research shows that patients diagnosed with left heart chamber enlargement often require a collaborative treatment strategy with their healthcare provider. This highlights the need for precise diagnostic methods. As healthcare evolves, integrating these advanced methodologies will be vital for improving patient outcomes and streamlining clinical workflows.
Outline Management and Treatment Strategies for Atrial Hypertrophy
Managing requires a comprehensive approach that includes several key strategies.
- : One of the primary features of effective management is . , dietary adjustments, and increased physical activity can significantly improve heart health. These modifications not only help reduce the strain on the heart but also play a role in preventing atrial hypertrophy, thereby enhancing overall well-being.
- : In addition to lifestyle changes, pharmacological treatments play a crucial role. Medications such as are often prescribed to manage related conditions like hypertension and atrial hypertrophy. These treatments help control symptoms and prevent complications, providing patients with a better quality of life.
- Surgical Interventions: For some patients, may be necessary. Procedures like catheter ablation or valve repair can address underlying causes of hypertrophy. These interventions can lead to significant improvements in heart function and patient outcomes.
- : Finally, are essential components of effective management. Regular assessments allow healthcare providers to evaluate treatment efficacy and make necessary adjustments. This proactive approach ensures that patients receive the best possible care tailored to their needs.

Conclusion
Atrial hypertrophy presents a significant clinical challenge, arising from the enlargement of heart chambers due to various underlying conditions. This condition is not just a structural change; it serves as a critical indicator of potential cardiovascular complications that can negatively impact patient health. Understanding the nuances of atrial hypertrophy is essential for healthcare providers, as it informs treatment strategies and enhances patient outcomes.
The article explored the causes and risk factors of atrial hypertrophy, highlighting the roles of:
- Hypertension
- Obesity
- Diabetes
Diagnostic techniques such as echocardiography and advanced ECG analysis were discussed, emphasizing their importance in timely identification and management. Effective management strategies, including:
- Lifestyle modifications
- Pharmacological treatments
- Surgical interventions
were outlined, showcasing the multifaceted approach required to address this condition.
Addressing atrial hypertrophy involves not only managing symptoms but also implementing preventive measures that can enhance heart health and quality of life. By focusing on lifestyle changes and utilizing advanced diagnostic tools, healthcare professionals can significantly reduce the risks associated with this condition. It is imperative for both patients and practitioners to remain vigilant and proactive in managing atrial hypertrophy, ensuring that cardiovascular health remains a priority in clinical practice.
Frequently Asked Questions
What is atrial hypertrophy?
Atrial hypertrophy refers to the enlargement of the heart's chamber areas, often resulting from prolonged pressure or volume overload.
Why is atrial hypertrophy clinically significant?
Atrial hypertrophy poses significant clinical challenges as it can lead to serious cardiovascular issues such as irregular heartbeat and heart failure. Recognizing hypertrophy is crucial for healthcare professionals as it signals underlying cardiac problems and influences treatment strategies.
What diagnostic tools are used to detect atrial hypertrophy?
Echocardiography and electrocardiograms (ECGs) are essential diagnostic tools used to reveal changes in chamber size and function related to atrial hypertrophy.
What challenges exist in traditional ECG interpretation?
Traditional ECG interpretation can be hindered by noise and artifacts that obscure critical data, making it difficult to assess heart chamber conditions accurately.
How does MaxYield™ improve ECG analysis?
MaxYield™ enhances ECG analysis by providing advanced noise filtering, distinct wave recognition, and rapid isolation of ECG waves from recordings affected by baseline wander, movement, and muscle artifact.
What types of ECG recordings can MaxYield™ salvage?
MaxYield™ can salvage previously obscured sections of lengthy Holter, 1-Lead, and patch monitor recordings.
What is the association between left heart chamber enlargement (LAE) and patient outcomes?
Left heart chamber enlargement (LAE) is associated with increased mortality and morbidity, making its detection vital in clinical practice. Patients with LAE often experience symptoms like breathlessness and fatigue.
What should doctors do regarding patients with LAE?
Doctors must investigate the underlying causes of LAE to help individuals manage symptoms and enhance their quality of life. Regular monitoring and management are essential for improving patient outcomes.