Introduction
Heart failure is a complex clinical syndrome that presents significant challenges to healthcare systems around the globe, and its prevalence continues to rise. Understanding the nuances of heart failure classification, particularly the critical role of ejection fraction (EF), is essential for effective management and improved patient outcomes. As medical professionals navigate the intricacies of treatment strategies, a key question emerges: how can a deeper comprehension of EF classifications enhance clinical decision-making and ultimately save lives?
By grasping the various EF classifications, healthcare providers can tailor treatment plans more effectively, leading to better patient care. This understanding not only aids in identifying the severity of heart failure but also informs the selection of appropriate therapies. As we delve deeper into the implications of EF in clinical practice, it becomes clear that enhancing our knowledge in this area can significantly impact patient outcomes.
Define Heart Failure and Ejection Fraction
, or heart failure (HF), is a clinical syndrome where the heart cannot pump enough blood to meet the body's metabolic demands. This condition can stem from various underlying issues, such as:
- coronary artery disease
- hypertension
- cardiomyopathy
A key measure in evaluating is the (EF), which indicates the percentage of blood ejected by the left ventricle with each heartbeat. Normal EF values typically range from 55% to 70%.
In cases of , the can be categorized as:
- preserved (HFpEF)
Each significantly impacts both and prognostic outcomes. Recent studies reveal that individuals with face a notably higher risk of readmission and mortality compared to those with . This highlights the critical importance of in clinical practice.
Furthermore, evolving definitions of emphasize the need for a dynamic understanding of EF trajectories. This understanding can better inform treatment decisions and .

Explore Heart Failure Classification Systems
Heart dysfunction classification plays a crucial role in managing individuals effectively, with the serving as a foundational element in this process. The NYHA system categorizes individuals into four classes based on their physical limitations:
- Class I indicates no symptoms
- Class II denotes mild symptoms
- Class III reflects marked limitations
- Class IV signifies symptoms at rest
This classification assists in tailoring treatment plans and monitoring disease progression effectively.
In addition to the NYHA classification, the American College of Cardiology/American Heart Association (ACC/AHA) classification further refines the . It distinguishes between the categories, including (HFrEF), mildly reduced ejection fraction (HFmrEF), and preserved ejection fraction (HFpEF). This dual classification system, which encompasses , is essential for understanding the underlying pathophysiology and guiding therapeutic interventions.
Recent studies have highlighted the limitations of the NYHA classification, particularly its weak correlation with cardiopulmonary exercise tests, which can lead to misclassification of individuals' functional capacity. For example, a secondary analysis of the PARADIGM-HF trial revealed that while higher correlate with worse prognoses, individuals in NYHA Class I with elevated NT-proBNP levels exhibited higher event rates than those with lower levels across all classes. This finding underscores the importance of considering additional biomarkers alongside functional classifications to and treatment efficacy.
The application of the NYHA classification in clinical settings has shown promise, with interdisciplinary teams utilizing it to improve therapy and track outcomes. Hospitals have integrated into electronic health records (EHRs), facilitating seamless data flow and enhancing care coordination. Insights from specialists emphasize the significance of these categories in guiding clinical decisions and improving patient education, ultimately leading to better health outcomes in .
Moreover, the lifetime risk of developing has increased to 24%, highlighting the need for effective management strategies. The could reach $858 billion by 2050, underscoring the economic implications of this condition and the necessity for precise classification systems. Additionally, patient engagement is vital, as are associated with lower hospitalizations and mortality. This emphasizes the importance for health tech developers to focus on enhancing healthcare delivery and patient outcomes. Furthermore, addressing racial disparities in cardiac mortality rates is essential for tailoring interventions and improving overall management.

Analyze the Role of Ejection Fraction in Clinical Practice
serves as a crucial metric in diagnosing and managing cardiac dysfunction. It helps clinicians categorize the condition using and . For patients with (HFrEF), which is defined as an EF of less than 40%, and beta-blockers are commonly prescribed. These medications aim to improve and reduce mortality rates. In contrast, patients with preserved (HFpEF), which is characterized by an EF of 50% or higher, typically require management strategies that focus on controlling comorbidities, such as hypertension and diabetes, rather than directly improving heart function.
is vital, as it offers valuable insights into disease progression and treatment effectiveness. Recent guidelines emphasize the importance of routine EF evaluations to inform clinical decisions and improve patient outcomes. For instance, the American College of Cardiology has updated its consensus pathways to include recommendations for regular EF assessments, particularly for individuals with varying symptoms or those undergoing changes in therapy.
Real-world examples illustrate how ejection rate influences treatment strategies. In a clinical setting, a patient with an EF of 35% may begin guideline-directed medical therapy (GDMT) aimed at enhancing . Meanwhile, another patient with an EF of 55% may focus on lifestyle modifications and managing related conditions. This tailored approach underscores the significance of , ensuring that patients receive the most appropriate and effective care.

Integrate Advanced ECG Analysis for Accurate Ejection Fraction Measurement
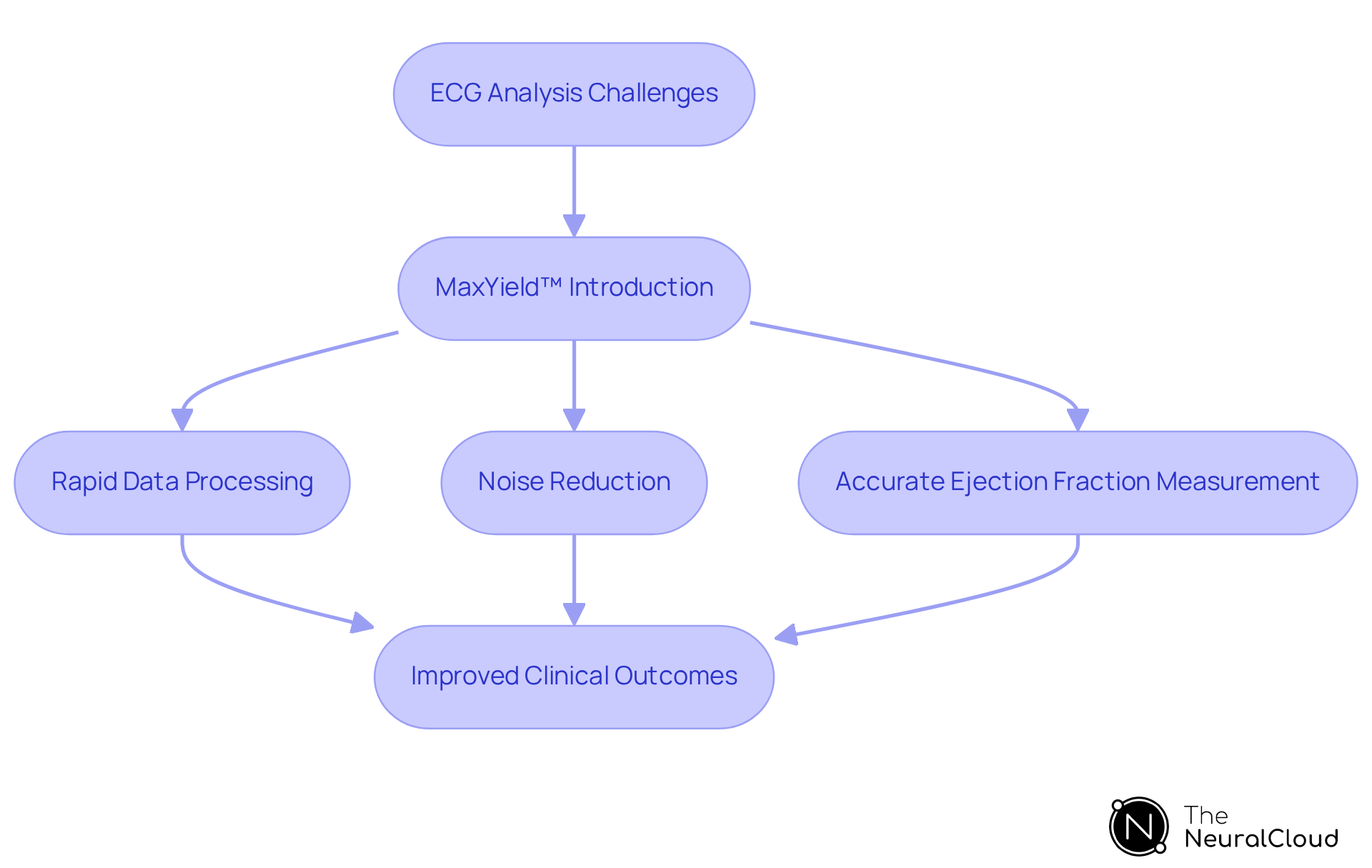
often faces challenges, particularly in achieving precise ejection measurements. Advanced technologies like Neural Cloud Solutions' address these issues effectively.
utilizes innovative AI algorithms to process ECG data rapidly and reliably. This platform identifies that are essential for . Notably, is device-agnostic, meaning it can capture ECG recordings from any 1-lead or 3-lead device. It can , .
The advantages of using are significant. By , rather than manual data processing. This shift ultimately leads to better clinical outcomes. Additionally, with its , MaxYield™ revolutionizes , providing clinicians with .
Conclusion
Understanding heart failure and the critical role of ejection fraction (EF) is essential for effective management and treatment of this complex condition. Accurate classification of heart failure, particularly through the lens of ejection fraction, informs therapeutic strategies and significantly impacts patient outcomes. By distinguishing between reduced and preserved ejection fractions, healthcare providers can tailor interventions to meet the specific needs of each patient, enhancing overall care.
Key insights highlight the necessity of adopting comprehensive classification systems like the New York Heart Association (NYHA) and the American College of Cardiology/American Heart Association (ACC/AHA) frameworks. These systems facilitate a deeper understanding of heart failure's nuances, allowing for more personalized treatment plans. Furthermore, the integration of advanced ECG technologies, such as Neural Cloud Solutions' MaxYield™, improves diagnostic accuracy and clinical efficiency, ultimately leading to better patient management.
Given the increasing prevalence of heart failure and its associated economic burden, healthcare professionals must stay informed about the latest classification systems and measurement techniques. Emphasizing the importance of ejection fraction in heart failure management aids in risk stratification and fosters a proactive approach to patient care. As the landscape of heart failure treatment evolves, embracing these insights will be crucial in improving outcomes and advancing the field of cardiology.
Frequently Asked Questions
What is heart failure (HF)?
Heart failure is a clinical syndrome where the heart cannot pump enough blood to meet the body's metabolic demands, often due to underlying issues such as coronary artery disease, hypertension, or cardiomyopathy.
What is ejection fraction (EF)?
Ejection fraction is a key measure in evaluating cardiac function, indicating the percentage of blood ejected by the left ventricle with each heartbeat. Normal EF values typically range from 55% to 70%.
How is ejection fraction categorized in heart failure?
Ejection fraction in heart failure can be categorized as reduced (HFrEF) or preserved (HFpEF), which significantly impacts treatment strategies and prognostic outcomes.
What are the risks associated with reduced ejection fraction (HFrEF)?
Individuals with reduced ejection fraction face a notably higher risk of readmission and mortality compared to those with preserved ejection fraction.
Why is accurate measurement of ejection fraction important?
Accurate measurement of ejection fraction is critical in clinical practice as it informs treatment decisions and enhances patient care.
How is the understanding of ejection fraction evolving in relation to cardiac dysfunction?
Evolving definitions of cardiac dysfunction emphasize the need for a dynamic understanding of ejection fraction trajectories to better inform treatment decisions and enhance care for patients.
List of Sources
- Define Heart Failure and Ejection Fraction
- Clinical trial offers first-of-its-kind heart failure treatment (https://health.ucdavis.edu/news/headlines/clinical-trial-offers-first-of-its-kind-heart-failure-treatment/2026/02)
- Cardiology Experts Warn of Growing Heart Failure Epidemic and Soaring Costs in New HF Stats 2025 Report | HFSA (https://hfsa.org/cardiology-experts-warn-growing-heart-failure-epidemic-and-soaring-costs-new-hf-stats-2025-report)
- Study finds high risk of readmission and death among heart failure patients (https://medicalxpress.com/news/2026-02-high-readmission-death-heart-failure.html)
- New Joint Scientific Statement on Ejection Fraction Released by Leading Heart Failure Organisations (https://escardio.org/news/press/press-releases/new-joint-scientific-statement-on-ejection-fraction-released-by-leading-heart-failure-organisations)
- Heart Failure Management: Current Approaches and Future Directions (https://thecardiologyadvisor.com/features/heart-failure-management-2026)
- Explore Heart Failure Classification Systems
- ajconline.org (https://ajconline.org/article/S0002-9149(08)01715-3/fulltext)
- Heart Failure Society of America (HFSA) Scientific Statement: Update on Device Based Therapies in Heart Failure (https://hfsa.org/hf-stats-2025-heart-failure-epidemiology-and-outcomes-statistics)
- Clinical trial offers first-of-its-kind heart failure treatment (https://health.ucdavis.edu/news/headlines/clinical-trial-offers-first-of-its-kind-heart-failure-treatment/2026/02)
- New Scientific Statement Guides Clinicians on How to Integrate Digital Health Tools Into Heart Failure Care | HFSA (https://hfsa.org/new-scientific-statement-guides-clinicians-how-integrate-digital-health-tools-heart-failure-care)
- New York Heart Association classification may be an incomplete predictor of adverse cardiovascular outcomes | 2 Minute Medicine (https://2minutemedicine.com/new-york-heart-association-classification-may-be-an-incomplete-predictor-of-adverse-cardiovascular-outcomes)
- Analyze the Role of Ejection Fraction in Clinical Practice
- Heart Failure Management: Current Approaches and Future Directions (https://thecardiologyadvisor.com/features/heart-failure-management-2026)
- New Joint Scientific Statement on Ejection Fraction Released by Leading Heart Failure Organisations (https://escardio.org/news/press/press-releases/new-joint-scientific-statement-on-ejection-fraction-released-by-leading-heart-failure-organisations)
- 125 Sayings And Quotes About Heart Disease (https://parade.com/1187612/michelle-parkerton/quotes-about-heart-disease)
- Heart Failure Epidemiology and Outcomes Statistics: A Report of the Heart Failure Society of America - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10864030)
- Integrate Advanced ECG Analysis for Accurate Ejection Fraction Measurement
- AccurKardia wins FDA clearance for next-generation ECG analysis system | Medical Economics (https://medicaleconomics.com/view/accurkardia-wins-fda-clearance-for-next-generation-ecg-analysis-system)
- 10 best quotes on AI from Becker’s CEO + CFO Roundtable (https://beckershospitalreview.com/healthcare-information-technology/ai/10-best-quotes-on-ai-from-beckers-ceo-cfo-roundtable)
- Overheard this week: 6 notable quotes on healthcare AI (https://healthexec.com/topics/patient-care/overheard-week-6-notable-quotes-healthcare-ai)
- My favorite AI in Healthcare quotes | AI Grand Rounds (https://linkedin.com/posts/ai-grand-rounds_my-favorite-ai-in-healthcare-quotes-activity-7275811766381527040-osDD)
- The diagnostic accuracy of artificial intelligence enhanced electrocardiography for the detection of cardiac dysfunction (https://explorationpub.com/Journals/ec/Article/101293)