Introduction
Understanding the intricacies of ST Elevation Myocardial Infarction (STEMI) is essential for healthcare professionals, as timely recognition can significantly influence patient outcomes. This guide explores the critical steps for analyzing ST elevation myocardial infarction ECGs, providing readers with the necessary knowledge to navigate the complexities of diagnosis and interpretation. Given the high stakes involved, it is important to identify common pitfalls in ECG analysis that may lead to misdiagnosis. Clinicians must be equipped with strategies to address these challenges effectively.
Understand the Basics of ST Elevation Myocardial Infarction (STEMI)
ST Elevation Myocardial Infarction (STEMI) is a critical condition characterized by the complete blockage of a coronary artery, leading to significant damage to the heart muscle. It is essential to recognize that elevation, particularly an elevation in the ST segment. This elevation signifies transmural ischemia, indicating that the heart muscle is deprived of oxygen due to the blockage.
Understanding STEMI, including its causes, symptoms, and potential complications, is vital for healthcare professionals involved in cardiac care, especially when analyzing the ECG. Common symptoms include:
- Chest pain
- Shortness of breath
- Sweating
All of which require immediate medical attention. Recent studies, such as those from the FAST-MI programme, reveal that heart attacks remain a significant concern, underscoring the necessity for timely intervention.
Moreover, STEMI has been identified as a serious condition, with a median duration of 12 days from symptom onset, complicating both diagnosis and treatment. Case studies demonstrate the effectiveness of technology, especially artificial intelligence, in identifying heart attacks, particularly through platforms like ECG analysis software, which automates the labeling of ECG waveforms and enhances signal clarity. This technology allows healthcare providers to concentrate on high-level decision-making, significantly improving clinical workflows and patient outcomes.
As our understanding of heart attacks continues to evolve, ongoing research into treatment options and their implications is crucial for refining treatment strategies.

Identify Key ECG Criteria for STEMI Diagnosis
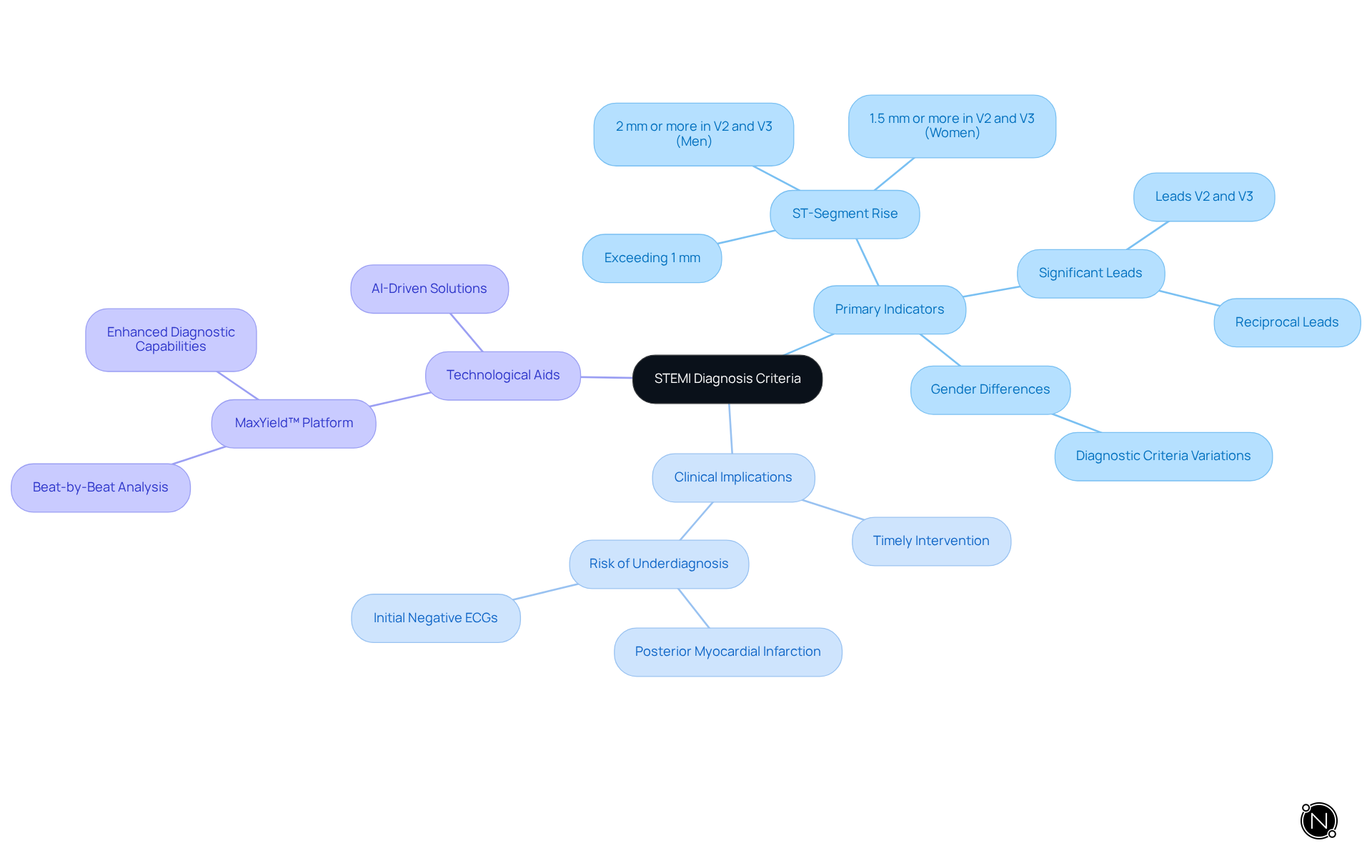
To diagnose STEMI, healthcare professionals must identify specific criteria. The primary indicator for STEMI is an ST-segment rise exceeding 1 mm in two or more adjacent recordings on a 12-channel ECG. For example, in leads V2 and V3, an ST-segment rise is particularly significant, with rises of 2 mm or more in men and 1.5 mm or more in women being diagnostic. Additionally, ST-segment elevation may occur in leads opposite those showing depression.
Clinicians must be familiar with these criteria to make informed decisions swiftly, as timely interventions can greatly improve patient outcomes. A recent study highlighted that 11% of patients ultimately diagnosed with a heart attack had an initial negative ECG, emphasizing the need for serial ECG testing. Furthermore, the 2025 American Heart Association/American College of Cardiology Guidelines stress the importance of early recognition, including ECG interpretation, in managing acute coronary syndromes.
It is also crucial to consider the risk of underdiagnosing posterior myocardial infarction (MI), which can complicate STEMI diagnosis. Utilizing advanced technologies like the ECG analysis software can aid healthcare professionals in accurately analyzing ECG data, thereby enhancing diagnostic accuracy.
Analyze ECG Readings for ST Elevation: A Step-by-Step Approach
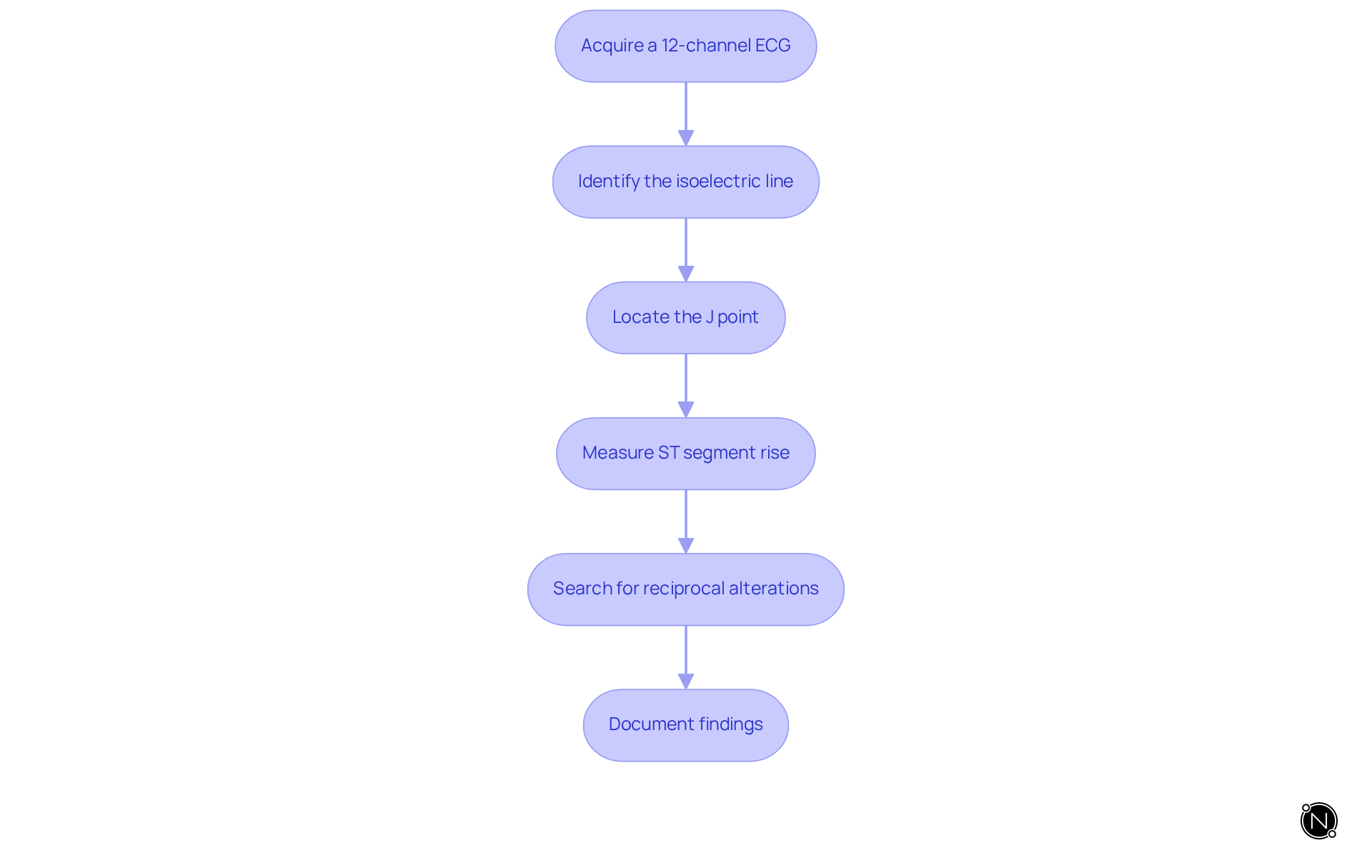
To effectively analyze ECG readings for ST elevation, follow these steps:
- Acquire a recording: Ensure that the ECG is recorded correctly, with all connections positioned accurately to capture a comprehensive view of the heart's electrical activity. Be mindful of common errors in lead placement, such as mispositioning of the limb leads or incorrect placement of precordial leads, as these can significantly affect the accuracy of the readings.
- Identify the baseline: This baseline level of the ECG is crucial for determining the degree of ST rise. Accurate identification is essential for reliable measurements.
- Locate the J point: This point marks the junction where the QRS complex transitions into the ST segment. Measure the ST segment from this critical point, ensuring that the assessment occurs 0.04 seconds after the J point for accurate measurement.
- Measure the ST elevation: Assess the increase in millimeters above the baseline in the pertinent electrodes. It is essential to compare these measurements with neighboring connections to verify the height and prevent misinterpretation.
- Search for reciprocal changes: Examine for ST segment depression in locations that are electrically opposite to those displaying an increase. This can provide additional support for a STEMI diagnosis, as reciprocal changes are often indicative of myocardial ischemia.
- Document findings: Clearly record your observations, noting any significant rises and the corresponding connections. Emphasizing the importance of thorough documentation is vital for subsequent diagnosis and patient management, ensuring that all relevant information is available for future reference.
By following these steps, healthcare professionals can enhance their skills related to ECG interpretation, leading to more accurate diagnoses and improved patient outcomes.
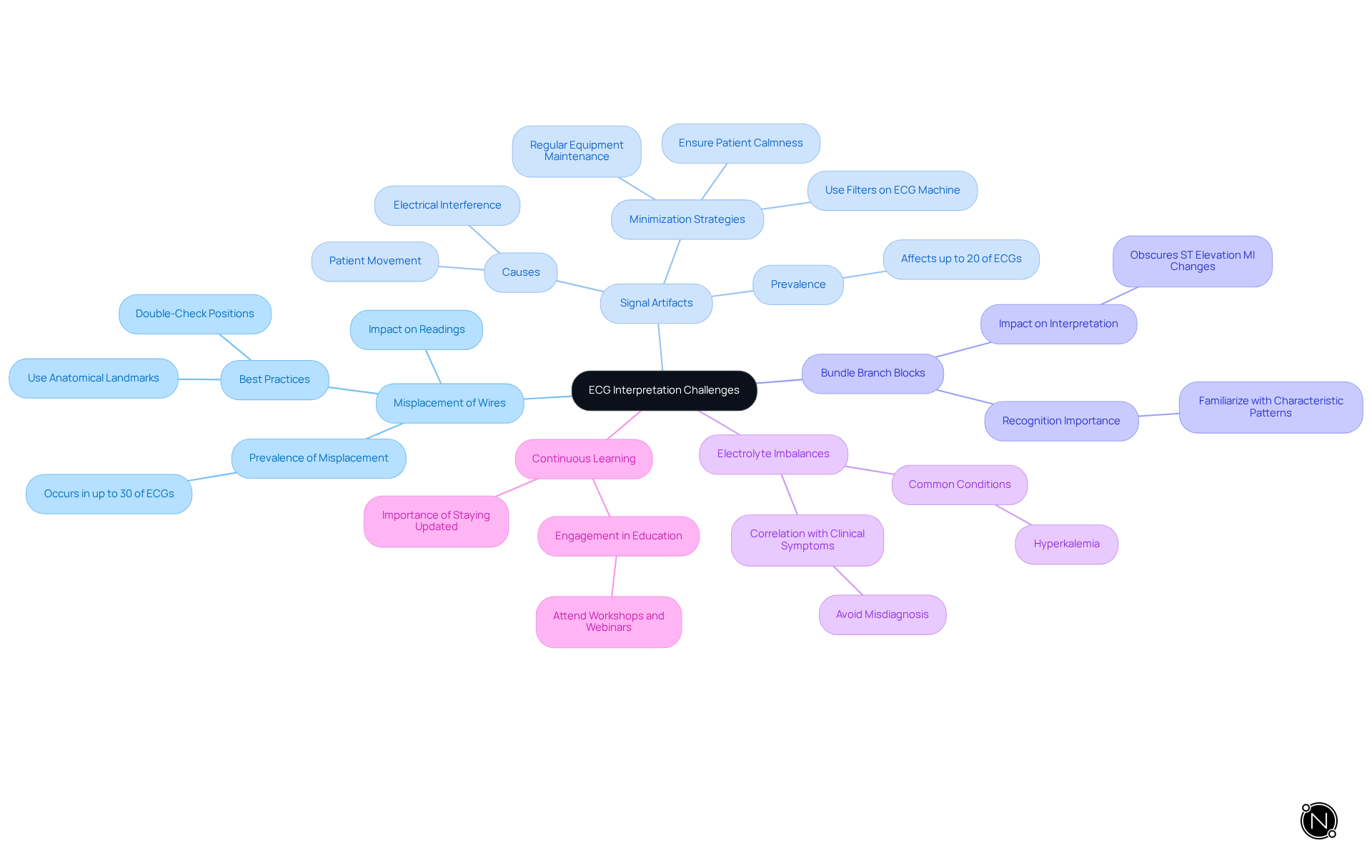
Troubleshoot Common ECG Interpretation Challenges
Interpreting ECGs can present several challenges. Common issues include misinterpretation, artifacts, patient movement, electrical interference, and the need for accurate lead placement. Addressing these challenges is crucial for effective diagnosis.
Precise positioning of wires is essential for dependable readings. Misplacement can lead to significant misinterpretations, such as false positives for myocardial infarction. A study found that misplacement occurs in up to 30% of ECGs, resulting in misdiagnoses. If misplacement is suspected, recheck the electrode positions and obtain a new ECG to ensure accuracy. Best practices include using anatomical landmarks for lead placement and double-checking positions before recording.
Electrical interference or patient movement can introduce artifacts that obscure true cardiac signals. Research indicates that artifacts can affect up to 20% of ECG recordings. To minimize these, ensure the patient is calm and that the ECG equipment is functioning properly. Regular maintenance and checks can help reduce the occurrence of artifacts. Additionally, consider using filters on the ECG machine to reduce noise.
Certain conditions can obscure changes, complicating the interpretation of potential myocardial infarction. Familiarize yourself with the characteristic patterns of these conditions to differentiate them from genuine changes. Cardiologists emphasize the importance of recognizing these patterns to avoid misinterpretation.
Conditions such as hyperkalemia can resemble a myocardial infarction on an ECG. Always correlate ECG findings with clinical symptoms and laboratory results to avoid misdiagnosis. For example, a cardiologist noted that misdiagnosing hyperkalemia as STEMI can lead to inappropriate treatment, highlighting the need for careful analysis.
The field of ECG interpretation is constantly evolving. Staying updated with the latest guidelines is essential for refining skills and knowledge, ensuring accurate interpretation of complex cases. Engaging in continuous education, such as attending workshops or webinars, can significantly enhance proficiency.
Conclusion
Mastering the analysis of ST Elevation Myocardial Infarction (STEMI) through ECG interpretation is essential for timely and effective patient care. This guide outlines the key components of understanding STEMI, from its definition and symptoms to the specific ECG criteria necessary for diagnosis. By grasping these fundamental concepts, healthcare professionals can improve their ability to recognize and respond to this critical condition.
Key insights discussed include:
- The importance of accurately identifying ST segment elevations
- Understanding the role of advanced technologies like the MaxYield™ platform
- Recognizing common challenges in ECG interpretation
By emphasizing a step-by-step approach to ECG analysis, the guide provides practical strategies for overcoming potential pitfalls, ensuring that healthcare providers can navigate the complexities of cardiac care with confidence.
In light of the ongoing evolution in cardiac care and the increasing prevalence of conditions like STEMI, continuous education and practice are essential. Engaging with the latest research and guidelines will not only refine diagnostic skills but also contribute to improved patient outcomes. It is imperative for healthcare professionals to remain vigilant and proactive in their approach to STEMI, as timely intervention can significantly alter the course of a patient's recovery.
Frequently Asked Questions
What is ST Elevation Myocardial Infarction (STEMI)?
STEMI is a critical condition characterized by the complete blockage of a coronary artery, leading to significant damage to the heart muscle.
What are the key ECG alterations associated with STEMI?
STEMI typically presents with distinct ECG alterations, particularly an ST elevation in the ST segment, which signifies transmural ischemia and indicates that the heart muscle is deprived of oxygen due to the blockage.
What are the common symptoms of STEMI?
Common symptoms of STEMI include chest pain, shortness of breath, and sweating, all of which require immediate medical attention.
What is the significance of the six-month mortality rates following heart attacks?
Recent studies reveal that six-month mortality rates following heart attacks remain a significant concern, highlighting the necessity for timely intervention.
How is STEMI related to COVID-19?
STEMI has been identified as a delayed complication of COVID-19, with a median duration of 12 days from symptom onset, complicating both diagnosis and treatment.
What role does advanced ECG analysis play in identifying STEMI?
Advanced ECG analysis, particularly through platforms like MaxYield™, automates the labeling of ECG waveforms and enhances signal clarity, allowing healthcare providers to focus on high-level decision-making and improve clinical workflows and patient outcomes.
Why is ongoing research into ST elevation MI ECG changes important?
Ongoing research into ST elevation MI ECG changes is crucial for refining treatment strategies as our understanding of heart attacks continues to evolve.
List of Sources
- Understand the Basics of ST Elevation Myocardial Infarction (STEMI)
- STEMI Archives - Cardiovascular News (https://cardiovascularnews.com/tag/stemi)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC8522676)
- tctmd.com (https://tctmd.com/news/should-we-be-looking-occlusion-mi-rather-stemi)
- Artificial intelligence may speed heart attack diagnosis and treatment (https://newsroom.heart.org/news/artificial-intelligence-may-speed-heart-attack-diagnosis-and-treatment)
- Identify Key ECG Criteria for STEMI Diagnosis
- tctmd.com (https://tctmd.com/news/ai-ecg-model-outperforms-stemi-criteria-identifying-acs-patients-occlusions)
- STEMI ECG Criteria: Key Insights into Ischemic ST-Elevation Patterns (https://powerfulmedical.com/blog/stemi-ecg-criteria)
- New Guideline on Acute Coronary Syndromes: Key Takeaways (https://consultqd.clevelandclinic.org/new-guideline-on-acute-coronary-syndromes-key-takeaways-for-cardiologists)
- medscape.com (https://medscape.com/viewarticle/top-updates-2025-acs-management-guidelines-2025a1000h6s)
- ACC, AHA Issue New Acute Coronary Syndromes Guideline - American College of Cardiology (https://acc.org/Latest-in-Cardiology/Journal-Scans/2025/02/27/17/01/ACC-AHA-Issue-New-Acute-Coronary-Syndromes-Guideline)
- Analyze ECG Readings for ST Elevation: A Step-by-Step Approach
- powerfulmedical.com (https://powerfulmedical.com/blog/announcing-the-ai-ecg-timi-study-a-multi-center-validation)
- acc.org (https://acc.org/About-ACC/Press-Releases/2025/03/29/17/21/AI-Model-Shows-High-Accuracy)
- STEMI ECG Criteria: Key Insights into Ischemic ST-Elevation Patterns (https://powerfulmedical.com/blog/stemi-ecg-criteria)
- tctmd.com (https://tctmd.com/news/ai-shows-promise-detecting-type-1-mi-and-need-revascularization)
- nature.com (https://nature.com/articles/s41746-024-01193-7)
- Troubleshoot Common ECG Interpretation Challenges
- Using AI to Detect ECG Abnormalities (https://nyit.edu/news/articles/using-ai-to-detect-ecg-abnormalities)
- tricog.com (https://tricog.com/reducing-ecg-diagnosis-time-with-tricogs-ai-driven-ecg-solutions?srsltid=AfmBOopiBxvsFMhfaDavNVKcb9GmHT_DkvRjBZ-DyyiIV5zFWtdThF_5)
- hssib.org.uk (https://hssib.org.uk/news-events-blog/report-highlights-concerning-variation-in-paramedic-ecg-education-and-training)
- newsandviews.aacvpr.org (https://newsandviews.aacvpr.org/Full-Article/electrocardiogram-interpretation-a-core-competency-cr-professionals-need-to-improve-care-outcomes-1)