Introduction
Understanding the landscape of ECG analysis is crucial for cardiologists, particularly in identifying critical conditions like ST-elevation myocardial infarction (STEMI). The MaxYield™ platform from Neural Cloud Solutions offers advanced technology that enhances the clarity and accuracy of ECG readings. This improvement can lead to better patient outcomes, addressing a significant challenge in the field.
Clinicians often face difficulties interpreting various ECG patterns associated with different types of STEMI. The MaxYield™ platform provides features that streamline this process, allowing for more effective diagnosis. By leveraging its capabilities, healthcare professionals can interpret ECG data with greater precision, ensuring timely and accurate assessments.
The advantages of using the MaxYield™ platform are clear. It not only improves the accuracy of ECG readings but also supports healthcare professionals in making informed decisions. This ultimately enhances patient care and outcomes, making it an essential tool in modern cardiology.
In this article, we will explore the essential ECG STEMI locations every cardiologist must know, delving into the nuances of each condition and the technological innovations that support better diagnostic practices.
Neural Cloud Solutions: MaxYield™ for Enhanced ECG Clarity
has long faced challenges, particularly in terms of clarity and accuracy. Neural Cloud Solutions addresses these issues with its technology, which automates the analysis of ECG signals through advanced algorithms and wave recognition. This innovative technology employs machine learning techniques to process ECG data swiftly, enabling healthcare professionals to make informed decisions based on accurate readings.
MaxYield™ boasts impressive capabilities, analyzing over 200,000 heartbeats in under five minutes. It provides beat-by-beat analysis that isolates and labels key features, including P-waves, QRS complexes, and T-wave intervals. By enhancing diagnostic accuracy, this platform is transforming cardiac care, making it invaluable for cardiologists and healthcare technicians.
Moreover, MaxYield™ is device-agnostic, seamlessly integrating with various ECG devices, such as 1-lead and 3-lead systems. This compatibility enhances workflow efficiency and productivity across the healthcare spectrum. The platform embodies advancements in noise filtering, ensuring the highest quality of ECG readings.
In summary, the MaxYield™ platform not only improves ECG clarity but also empowers healthcare professionals with the tools they need to deliver better patient care.

Anterior STEMI: Key ECG Patterns and Localization
Anterior STEMI is marked by ST-segment elevation, indicating a potential blockage of the left anterior descending artery (LAD). Clinicians should also be vigilant for leads II, III, aVF, which serves as an additional diagnostic indicator.
Recognizing these ECG patterns is crucial for determining the presence of myocardial infarction, as anterior STEMI is associated with a higher risk of complications. Recent studies highlight that timely intervention can significantly improve outcomes, underscoring the need for these vital ECG alterations.
Prominent cardiologists emphasize that early recognition for anterior STEMI is essential for optimizing treatment and improving survival rates.

Inferior STEMI: Diagnostic Criteria and Common Pitfalls
Inferior STEMI is primarily identified by ST elevation, along with reciprocal ST-segment depression in leads I and aVL. However, diagnosing this condition can be challenging due to the risk of misinterpretation, especially when patterns overlap with conditions like right ventricular infarction. For example, studies show that 1.4% of individuals diagnosed with STEMI were misdiagnosed. This highlights the importance for clinicians to remain vigilant in evaluating both clinical context and ECG findings. Misdiagnosis can lead to delayed treatment, which can be particularly harmful; patients experiencing longer delays often face worse outcomes.
Understanding the implications of ST elevation in these electrodes is crucial for detecting inferior STEMI to ensure timely intervention, which significantly enhances survival rates. The software from Neural Cloud Solutions addresses these challenges by automating ECG labeling and providing accurate interpretations. This not only helps reduce the risk of misdiagnosis but also lowers operational costs.
Features of MaxYield™:
- Automated ECG labeling
Advantages for Healthcare Professionals:
- Lowers operational costs
Enhanced training in ECG interpretation and awareness of atypical presentations can further minimize the risk of misdiagnosis, ultimately leading to improved patient outcomes. By leveraging the technology, healthcare professionals can improve their diagnostic accuracy and ensure timely treatment.

Posterior STEMI: Recognizing ECG Characteristics
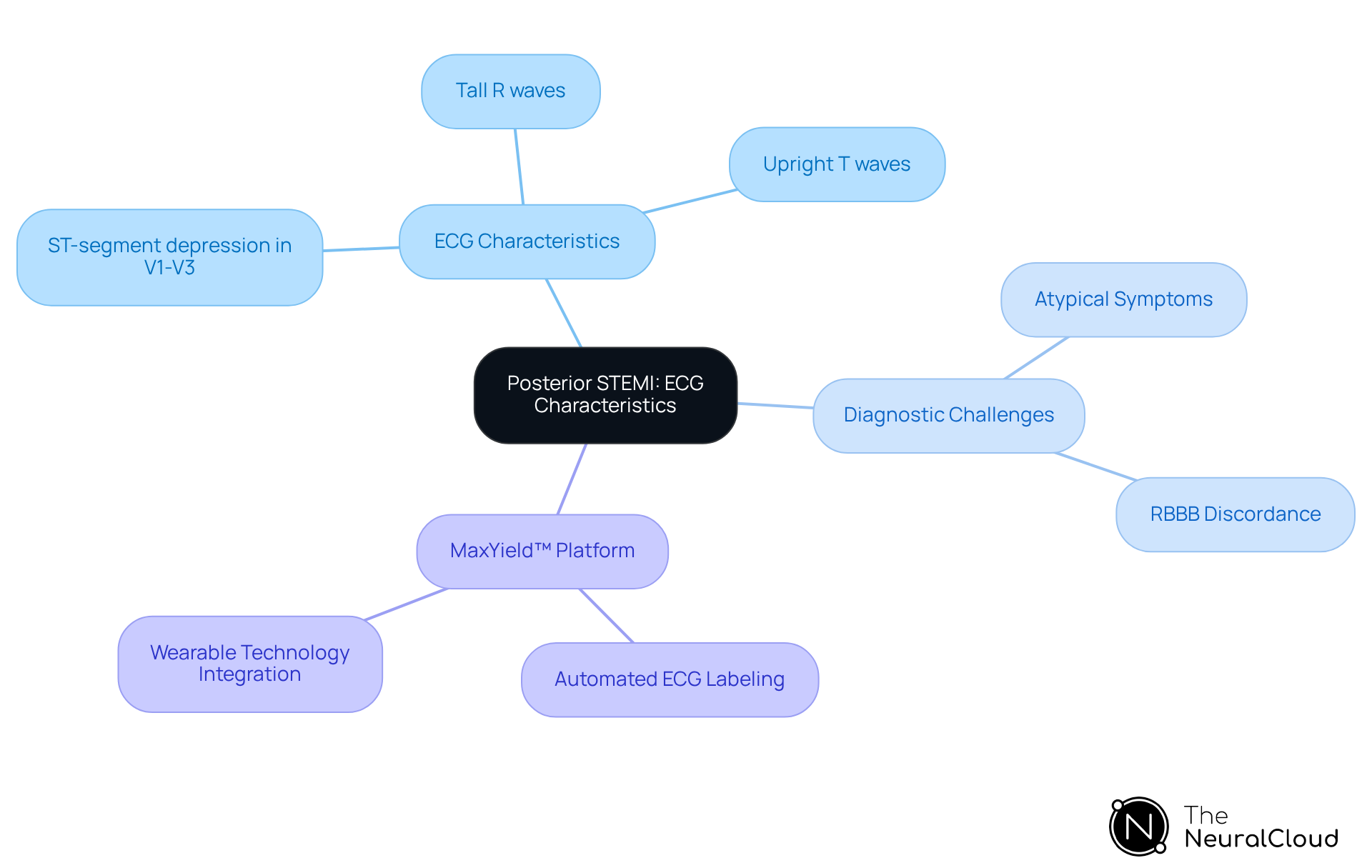
Posterior STEMI is identified by ST-segment depression in leads V1 to V3, along with tall, broad R waves and upright T waves in these areas. The diagnosis is confirmed through leads V7 to V9. Clinicians should be aware that posterior STEMI can present with atypical symptoms, complicating its identification, especially in patients showing signs of inferior myocardial infarction. Early recognition is vital, as it can significantly impact treatment outcomes.
Case studies illustrate the challenges in diagnosing posterior STEMI, particularly in the presence of right bundle branch block (RBBB), where notable discordance in ST-segment changes may indicate underlying myocardial infarction. The importance of prompt management is underscored by findings that highlight the risks of delayed treatment, emphasizing the need for swift evaluation and action in suspected cases of posterior STEMI.
Neural Cloud Solutions' technology addresses these challenges by automating ECG labeling and data extraction. This feature allows clinicians to focus their time and energy on tasks that require human expertise. By integrating with MaxYield™, healthcare providers can enhance the accuracy and reliability of ECG analysis while also reducing operational costs associated with manual data handling.
The benefits of the technology are clear: it streamlines the diagnostic process, improves diagnostic accuracy, and ultimately supports better patient outcomes. As Charle Viljoen states, 'Accurate diagnosis of heart attack permits the prompt initiation of suitable treatment,' highlighting the critical role of efficient management in healthcare.
Lateral STEMI: ECG Patterns and Diagnostic Importance
Lateral STEMI is marked by changes in leads I, aVL, V5, and V6, often accompanied by changes in the inferior leads (III and aVF). This specific ECG pattern typically indicates occlusion of the circumflex artery, which is involved in about 15% to 20% of all myocardial infarctions. Clinicians must be vigilant in recognizing these changes, as lateral STEMI can easily be mistaken for other cardiac conditions, leading to misdiagnosis. Early recognition is crucial for timely intervention, as delays in treatment can lead to significant morbidity and adverse outcomes.
Recent studies highlight the importance of technology in improving the diagnostic accuracy of ECG interpretation. For example, the Queen of Hearts AI-ECG platform has shown superior sensitivity (92%) and specificity (81%) compared to traditional methods. This advancement has significantly reduced the rate of misdiagnosis from 41.8% to 7.9%. Such improvements underscore the vital role of technology in enhancing clinical decision-making and treatment timelines.
Looking ahead to 2026, the integration of AI in detecting lateral heart attacks is expected to further refine diagnostic procedures. This will enable healthcare professionals to swiftly identify individuals in need of urgent care. As emergency medicine evolves, the emphasis on precise ECG interpretation remains essential, particularly for conditions like STEMI that may present with subtler symptoms. The ongoing development of AI tools aims to tackle these challenges, ultimately enhancing patient outcomes and resource management in emergency settings.

Right Ventricular STEMI: ECG Findings and Management
Right ventricular myocardial infarction (RVMI) is often associated with inferior myocardial infarction and can be identified by specific ECG changes. Clinicians should also monitor for ST-segment elevation in leads II, III, and aVF, as well as reciprocal ST-segment depression in the lateral leads. Recognizing RVMI is essential, as it can significantly impact hemodynamics and treatment strategies.
The technology from Neural Cloud Solutions addresses the challenges in ECG interpretation by providing advanced noise filtering and distinct wave recognition. This technology enhances the analysis, allowing clinicians to isolate critical data quickly, even in recordings affected by high levels of noise and artifact. As a result, RVMI can be identified promptly, improving patient outcomes.
The benefits of using the advanced technology are substantial. It not only streamlines the process but also supports clinicians in making informed decisions. Effective management of RVMI may require timely interventions to prevent severe complications, and the technology equips clinicians with the tools necessary to navigate these challenges effectively.

STEMI Diagnosis with Baseline ECG Abnormalities
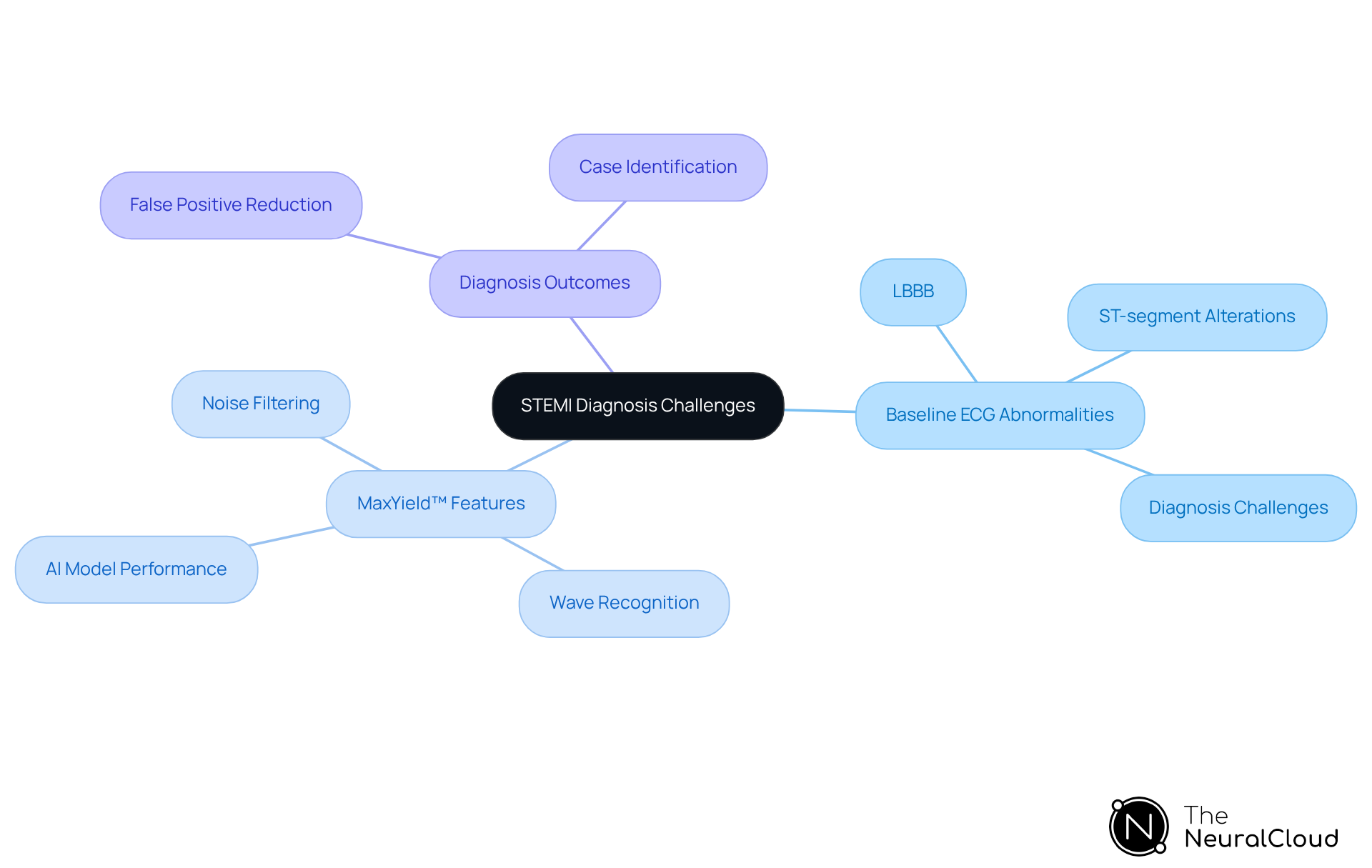
Baseline ECG irregularities, such as left bundle branch block (LBBB) and pre-existing ST-segment alterations, pose significant challenges in diagnosing ST-Elevation Myocardial Infarction (STEMI). Clinicians face the critical task of distinguishing between new changes indicative of myocardial injury and chronic alterations that could mislead diagnosis. Recent studies indicate that LBBB can obscure the detection of myocardial ischemia with ST elevation, with approximately 30% of left anterior descending (LAD) occlusions showing no ST elevation. This situation necessitates vigilance to ensure accurate diagnosis.
The MaxYield™ platform offers features that enhance ECG interpretation, including advanced algorithms and real-time analysis. These tools improve the clarity of ECG readings, enabling healthcare professionals to identify critical changes even amidst baseline conditions. The AI model within MaxYield™ has demonstrated superior performance compared to standard triage techniques, achieving higher accuracy, while conventional methods detected only 427 cases. This advancement significantly reduces diagnostic errors, lowering the rate from nearly 42% to around 8%.
By automating repetitive tasks and streamlining workflows, MaxYield™ supports clinicians in managing complex ECG interpretations more efficiently. Understanding the relationship between chronic ECG changes and acute coronary syndrome is vital for timely and effective patient management, ultimately enhancing outcomes in emergency care. As Bryn Mumma emphasizes, 'in emergency medicine, where every minute matters,' highlighting the urgency of accurate diagnosis.
STEMI vs. Occlusion MI: Key Diagnostic Criteria
Distinguishing between STEMI and occlusion myocardial infarction (OMI) is crucial, as OMI may not always show the typical ST-segment elevation associated with myocardial infarction. While STEMI is characterized by significant ST-segment elevation in specific leads, OMI can manifest through patterns that are often overlooked. Recent studies reveal that early recognition of OMI, which can lead to increased mortality rates if not quickly identified and treated.
Clinicians must remain updated on the evolving understanding of OMI equivalents, which encompass various ECG patterns that do not conform to traditional STEMI criteria. For instance, ST elevation was observed in 83% of OMI patients, while 82% exhibited reciprocal ST depression or T-wave inversion. These findings highlight the importance of thorough ECG analysis to ensure accurate diagnosis and timely intervention.
The diagnostic criteria for OMI have been refined, underscoring the necessity of considering clinical context alongside ECG findings. Clinical indicators, such as persistent ischemic symptoms and hemodynamic instability, should prompt immediate evaluation for reperfusion therapy. Case studies indicate that 55% of OMI patients were identified a median of 1.5 hours earlier using advanced ECG findings compared to conventional criteria, emphasizing the potential for improved outcomes through prompt intervention.
As the medical community increasingly acknowledges the OMI paradigm, emergency departments are urged to adopt updated diagnostic protocols. This shift not only enhances diagnostic precision but also aligns with current guidelines advocating for immediate angiography in high-risk individuals, regardless of whether they meet traditional heart attack criteria. The technology from Neural Cloud Solutions employs machine learning and automated labeling to significantly improve the efficiency of ECG analysis, addressing challenges like physiological variability and signal artifacts. Its continuous learning model ensures that diagnostic capabilities evolve with each use, further enhancing accuracy over time. Dr. Pendell Myers has emphasized the rationale for this paradigm shift, noting that many NSTEMI patients were later found to have complete coronary occlusion, necessitating a change in approach.

Traditional STEMI Criteria: Understanding Millimetric Thresholds
Traditional STEMI criteria state that a significant elevation in ST segments is necessary for diagnosis. For men under 40, this threshold increases to 2.5 mm in positions V2 or V3, while women require a minimum of 1.5 mm. Understanding these millimetric thresholds is crucial for accurate diagnosis and prompt treatment of myocardial infarction. However, recent findings suggest that these criteria may not cover all cases, especially among diverse populations.
Studies reveal disparities in diagnosis, with some groups showing rates as high as 27.5%. This highlights the need for clinicians to be aware of the limitations. Relying solely on traditional criteria could result in both misdiagnosis and delayed treatment, particularly in non-Western populations. As guidelines evolve, it is essential to consider these factors to enhance diagnostic accuracy and improve health outcomes.

Shark Fin Pattern: A Critical Indicator in STEMI Diagnosis
The shark fin pattern is a rare yet critical ECG finding that indicates severe myocardial ischemia. This distinctive waveform, resembling a shark fin, results from the fusion of the QRS complex, ST segment, and T waves. Recognition is vital, as it signifies a substantial burden of cardiac stress and demands immediate intervention. Clinicians must remain vigilant, given its association with high rates of in-hospital mortality and the necessity for urgent treatment.
Studies show that individuals exhibiting the shark fin pattern face an increased risk of adverse cardiac events. This underscores the importance of prompt recognition and treatment. With the integration of advanced algorithms, clinicians can identify this critical pattern. The technology effectively filters noise and isolates ECG waves, even in challenging recordings.
For instance, a case series highlighted that one adult individual with this pattern underwent percutaneous coronary intervention, while another developed malignant arrhythmias, leading to sudden cardiac death. Moza Guyanto emphasizes that when this pattern is identified, prompt and aggressive management is essential to enhance survival outcomes. Such outcomes highlight the need for clinicians to prioritize the identification of the shark fin pattern in their clinical practice.
Timely intervention, supported by advanced technologies like artificial intelligence, which evolves with each use to maximize diagnostic yield, can significantly impact patient survival and management. By utilizing these tools, clinicians can improve their capabilities, ultimately leading to better patient outcomes.

Conclusion
Understanding the essential ECG STEMI locations is crucial for cardiologists aiming to optimize patient outcomes in acute care settings. The article highlights the importance of accurately identifying specific ECG patterns associated with various types of myocardial infarction, including:
- Anterior STEMI
- Inferior STEMI
- Posterior STEMI
- Lateral STEMI
- Right ventricular STEMI
By leveraging advanced technologies like Neural Cloud Solutions' MaxYield™ platform, healthcare professionals can enhance their diagnostic capabilities, ensuring timely and effective interventions.
Key insights from the article emphasize the need for clinicians to be proficient in recognizing the distinct ECG characteristics of each STEMI type, as well as the potential pitfalls in diagnosis, such as:
- Baseline ECG abnormalities
- Subtle presentations of occlusion myocardial infarction
The integration of AI-driven tools not only aids in accurate ECG interpretation but also streamlines workflows, reducing the risk of misdiagnosis and improving overall patient care.
As the landscape of emergency medicine evolves, the emphasis on precise ECG analysis remains paramount. By embracing innovative technologies and continuous education in ECG interpretation, healthcare professionals can significantly impact survival rates and improve treatment outcomes for patients experiencing myocardial infarction. Prioritizing these advancements is essential for the future of cardiac care, ensuring that every minute counts in the critical moments of diagnosis and intervention.
Frequently Asked Questions
What is the MaxYield™ platform?
MaxYield™ is a platform developed by Neural Cloud Solutions that automates the analysis of ECG signals using advanced noise filtering and wave recognition technologies, enabling healthcare professionals to gain precise cardiac insights quickly.
How does MaxYield™ improve ECG analysis?
MaxYield™ enhances ECG analysis by analyzing over 200,000 heartbeats in under five minutes, providing beat-by-beat analysis that isolates and labels key features such as P-waves, QRS complexes, and T-wave intervals, transforming noisy recordings into detailed insights.
Is MaxYield™ compatible with various ECG devices?
Yes, MaxYield™ is device-agnostic and can seamlessly integrate with different ECG devices, including 1-lead and 3-lead systems, which enhances workflow efficiency and productivity in healthcare settings.
What are the key ECG patterns associated with anterior STEMI?
Anterior STEMI is characterized by ST-segment elevation in leads V1 to V4 and may also show reciprocal ST-segment depression in the inferior leads (II, III, aVF), indicating a potential blockage of the left anterior descending artery (LAD).
Why is early detection of anterior STEMI important?
Early detection of anterior STEMI is crucial as it is associated with a higher risk of complications and mortality. Prompt recognition can lead to better patient outcomes, making it essential for cardiologists to interpret these ECG changes accurately.
What are the diagnostic criteria for inferior STEMI?
Inferior STEMI is primarily identified by ST-segment elevation in leads II, III, and aVF, along with reciprocal ST-segment depression in leads I and aVL.
What challenges exist in diagnosing inferior STEMI?
Diagnosing inferior STEMI can be challenging due to the risk of misinterpretation, especially when ECG patterns overlap with conditions like right ventricular infarction, which can lead to treatment delays and worse patient outcomes.
How does MaxYield™ help reduce the risk of misdiagnosis?
MaxYield™ assists in reducing the risk of misdiagnosis through automated ECG labeling and advanced signal processing capabilities, enabling more accurate and timely diagnostics.
What advantages does MaxYield™ offer to healthcare professionals?
MaxYield™ reduces the risk of misdiagnosis, lowers operational costs, and enhances the ability of healthcare professionals to deliver timely and accurate treatment for patients.
List of Sources
- Neural Cloud Solutions: MaxYield™ for Enhanced ECG Clarity
- Automated ECG Report as a Factor in the Clinical Decision Pathway for Acute Chest Pain in the Emergency Department (https://cureus.com/articles/456496-automated-ecg-report-as-a-factor-in-the-clinical-decision-pathway-for-acute-chest-pain-in-the-emergency-department)
- Performance of an artificial intelligence-powered smartphone application in the UK clinical settings: ECG automation compared to healthcare professionals - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12532542)
- stocktitan.net (https://stocktitan.net/news/AIMLF/aiml-subsidiary-neural-cloud-signs-non-binding-agreement-with-9gt8a327pgvx.html)
- Current and Future Use of Artificial Intelligence in Electrocardiography - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10145690)
- Automated ECG Analysis Software Market Analysis: Identifying key issues and market drivers for strategic business planning at growth rate of 12% from (https://linkedin.com/pulse/automated-ecg-analysis-software-market-identifying-key-1fxre)
- Anterior STEMI: Key ECG Patterns and Localization
- Cover Story | Acute Coronary Syndromes: New Perspectives, New Data - American College of Cardiology (https://acc.org/Latest-in-Cardiology/Articles/2024/06/01/01/42/Cover-Story-Acute-Coronary-Syndromes-New-Perspectives-New-Data)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC4193075)
- Anterior Myocardial Infarction (https://litfl.com/anterior-myocardial-infarction-ecg-library)
- Trends and Outcomes of ST‐Segment–Elevation Myocardial Infarction Among Young Women in the United States | Journal of the American Heart Association (https://ahajournals.org/doi/10.1161/JAHA.122.026811)
- STEMI - Electrocardiogram - M3 Curriculum | SAEM (https://saem.org/about-saem/academies-interest-groups-affiliates2/cdem/for-students/online-education/m3-curriculum/group-electrocardiogram-(ecg)-rhythm-recognition/stemi)
- Inferior STEMI: Diagnostic Criteria and Common Pitfalls
- Diagnosis and Management of an Inferior ST-elevation Myocardial Infarction: A Simulation Scenario - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6443514)
- Delays in STEMI Cardiogenic Shock Care Come at a Cost: DanGer Shock (https://tctmd.com/news/delays-stemi-cardiogenic-shock-care-come-cost-danger-shock)
- Top 5 MI ECG Patterns You Must Know (https://healio.com/cardiology/learn-the-heart/ecg-review/ecg-interpretation-tutorial/stemi-mi-ecg-pattern)
- Incidence, relevant patient factors, and clinical outcomes of the misdiagnosis of ST-elevation myocardial infarction: Results from the Korea Acute Myocardial Infraction Registry (https://esc365.escardio.org/journal/68557)
- Misdiagnosis of Acute Myocardial Infarction: A Systematic Review of the Literature - PubMed (https://pubmed.ncbi.nlm.nih.gov/33606411)
- Posterior STEMI: Recognizing ECG Characteristics
- Recognition and management of posterior myocardial infarction: a retrospective cohort study - The British Journal of Cardiology (https://bjcardio.co.uk/2017/04/recognition-and-management-of-posterior-myocardial-infarction-a-retrospective-cohort-study)
- Posterior infarction: a STEMI easily missed - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8762803)
- ECG Case: Posterior STEMI — Manitoba ACS Network (https://mbacsnetwork.ca/newsletter-issues/ecg-case-posterior-stemi)
- Case report: Posterior myocardial infarction in presence of right bundle branch block: an old concept with new findings - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6177014)
- Delays in STEMI Cardiogenic Shock Care Come at a Cost: DanGer Shock (https://tctmd.com/news/delays-stemi-cardiogenic-shock-care-come-cost-danger-shock)
- Lateral STEMI: ECG Patterns and Diagnostic Importance
- AI-ECG Finds STEMI Faster, Cuts False-Positive Cath Lab Activations (https://tctmd.com/news/ai-ecg-finds-stemi-faster-cuts-false-positive-cath-lab-activations)
- Lateral Wall Myocardial Infarction - StatPearls - NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK537228)
- STEMI Diagnosis with Baseline ECG Abnormalities
- Thoughts about the abnormalities in the electrocardiogram of patients with acute myocardial infarction with emphasis on a more accurate method of interpreting ST-segment displacement: part I - PubMed (https://pubmed.ncbi.nlm.nih.gov/17680618)
- Impact of baseline ECG characteristics on changes in cardiac biomarkers and echocardiographic metrices after acute myocardial infarction treated with Empagliflozin - Scientific Reports (https://nature.com/articles/s41598-024-64175-5)
- litfl.com (https://litfl.com/omi-replacing-the-stemi-misnomer)
- AI-ECG Finds STEMI Faster, Cuts False-Positive Cath Lab Activations (https://tctmd.com/news/ai-ecg-finds-stemi-faster-cuts-false-positive-cath-lab-activations)
- New study finds AI model improves heart attack detection (https://health.ucdavis.edu/news/headlines/new-study-finds-ai-model-improves-heart-attack-detection/2025/11)
- STEMI vs. Occlusion MI: Key Diagnostic Criteria
- rebelem.com (https://rebelem.com/upping-our-ecg-game-omi-vs-stemi)
- From STEMI to occlusion MI: paradigm shift and ED quality improvement - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9001399)
- Checking your browser - reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC8065286)
- A New Approach to Acute Coronary Syndromes: Occlusion MI (OMI) vs. Non-Occlusion MI (NOMI) – The Cardiovascular (https://ecgwaves.com/topic/a-new-approach-to-acute-coronary-syndromes-occlusion-mi-omi-vs-non-occlusion-mi-nomi)
- ACS guidelines 2025 - The OMI has officially arrived! - ED Guidelines (https://edguidelines.com/acs-guidelines-2025-the-omi-has-officially-arrived)
- Traditional STEMI Criteria: Understanding Millimetric Thresholds
- STEMI ECG Criteria: Key Insights into Ischemic ST-Elevation Patterns (https://powerfulmedical.com/blog/stemi-ecg-criteria)
- ahajournals.org (https://ahajournals.org/doi/10.1161/JAHA.119.015477)
- journalmc.org (https://journalmc.org/index.php/JMC/article/view/3939/3285)
- Trends and Outcomes of ST‐Segment–Elevation Myocardial Infarction Among Young Women in the United States | Journal of the American Heart Association (https://ahajournals.org/doi/10.1161/JAHA.122.026811)
- Prevalence of ECGs Exceeding Thresholds for ST-Segment-Elevation Myocardial Infarction in Apparently Healthy Individuals: The Role of Ethnicity - PubMed (https://pubmed.ncbi.nlm.nih.gov/32573319)
- Shark Fin Pattern: A Critical Indicator in STEMI Diagnosis
- Decoding the Shark Fin EKG: Recognizing STEMI Patterns (https://oreateai.com/blog/decoding-the-shark-fin-ekg-recognizing-stemi-patterns/a43bdf097b0c0dec3f3238ac7ec6298c)
- THE SHARK FIN PATTERN AS A PREDICTOR OF SUDDEN CARDIAC DEATH IN ISCHEMIC AND NON-ISCHEMIC PATIENTS | Indonesian Global Journal Of Medical Research and Development (https://ejournal.uigm.ac.id/index.php/IGJMRD/article/view/6645)
- 5 Cardiology Headlines You Missed in January 2026 | HCPLive (https://hcplive.com/view/5-cardiology-headlines-you-missed-in-january-2026)
- Shark Fin Electrocardiogram: A Deadly Electrocardiogram Pattern in ST-Elevation Myocardial Infarction (STEMI) - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8317974)